Today’s waiting list data reveals some of the startling challenges before us. Following the publication of the elective recovery plan earlier this week, it’s unsurprising that we see yet another record waiting list finally topping 6 million. However, diving into the figures reveals a number of worrying trends.
- Many more people are waiting much longer than previously. It’s not just those at the end of the tail.
- The rise in waiting list is down to lower activity levels, not a surge in people returning to seek care.
- At 2019 levels, we would have expected to see 8 million more people joining the waiting list than have been referred since the pandemic.
- The pressures we’re seeing now are just a prelude to what we’ll see when those people return.
Taken together this means that the challenge of managing those on the waiting list is about to get much more difficult.
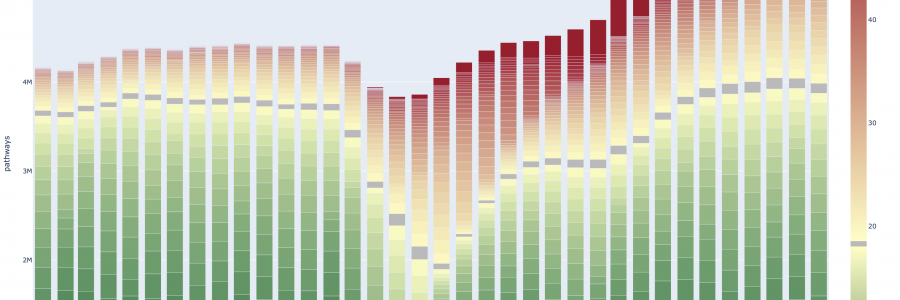
The chart below shows just how waiting duration has changed during the pandemic.
The columns show how long people have been waiting each week since the beginning of 2019. The grey lines show the number of people waiting just over 18 weeks. Above that and they’ve waited longer. Increasingly, much longer.
The graph shows that the number of people waiting below 18 weeks is broadly what it was in pre-pandemic days. But we now have another 2.2million people on top of that who’ve already waited over 18 weeks.
While the media has often focused on the people at the extreme tail of the waiting list, this graph shows the scale of the problem with a large number waiting a lot longer than in the past, though thankfully for them, not as long as the 310,000 waiting for over a year.
These are people who’ll need much more support than we’ve historically provided to people while they’re waiting for substantive treatment to begin.
So what to do? Well many of the measures in the elective recovery plan make sense. It’s certainly right to increase capacity. However, without radical changes to make the most of every possible efficiency and to help patients manage their care while they wait, we’re going to struggle.
The DHC welcomes the focus on digital in the elective recovery plan. Virtual wards, managing pathways more effectively, triaging and a greater utilisation of AI will all help.
But there’s always a danger of losing focus. We need to learn from what’s gone well, what’s been less successful and why other countries seem to be faring better.
Specifically, we need to measure and incentivise effective interventions that improve overall outcomes. Too often NHS procurements have a history of buying against over-specified details, while avoiding incentivising changes that have a significant impact on outcomes.
With a new focus on elective recovery, let’s make sure we avoid repeating past mistakes and incentivise results.